Hip Injections for Arthritis: Types, Cost
Compare all hip injection types for arthritis: cortisone, gel (HA), PRP, and stem cell. Costs, Medicare coverage, and which works best.
By Joint Pain Authority Team
Quick Answer
Four types of injections are used for hip arthritis: cortisone (most common, covered by Medicare, provides 4-12 weeks of relief), hyaluronic acid/gel injections (off-label for hip, growing evidence, 3-6 months of relief), PRP (emerging, not covered by insurance, $500-$1,500), and stem cell therapy (experimental, not covered, $3,000-$8,000). Imaging guidance is essential for all hip injections because the joint is deep. Cortisone is the typical starting point, with HA injections as the next step for patients wanting longer-lasting relief.
Why Hip Injections Are Different
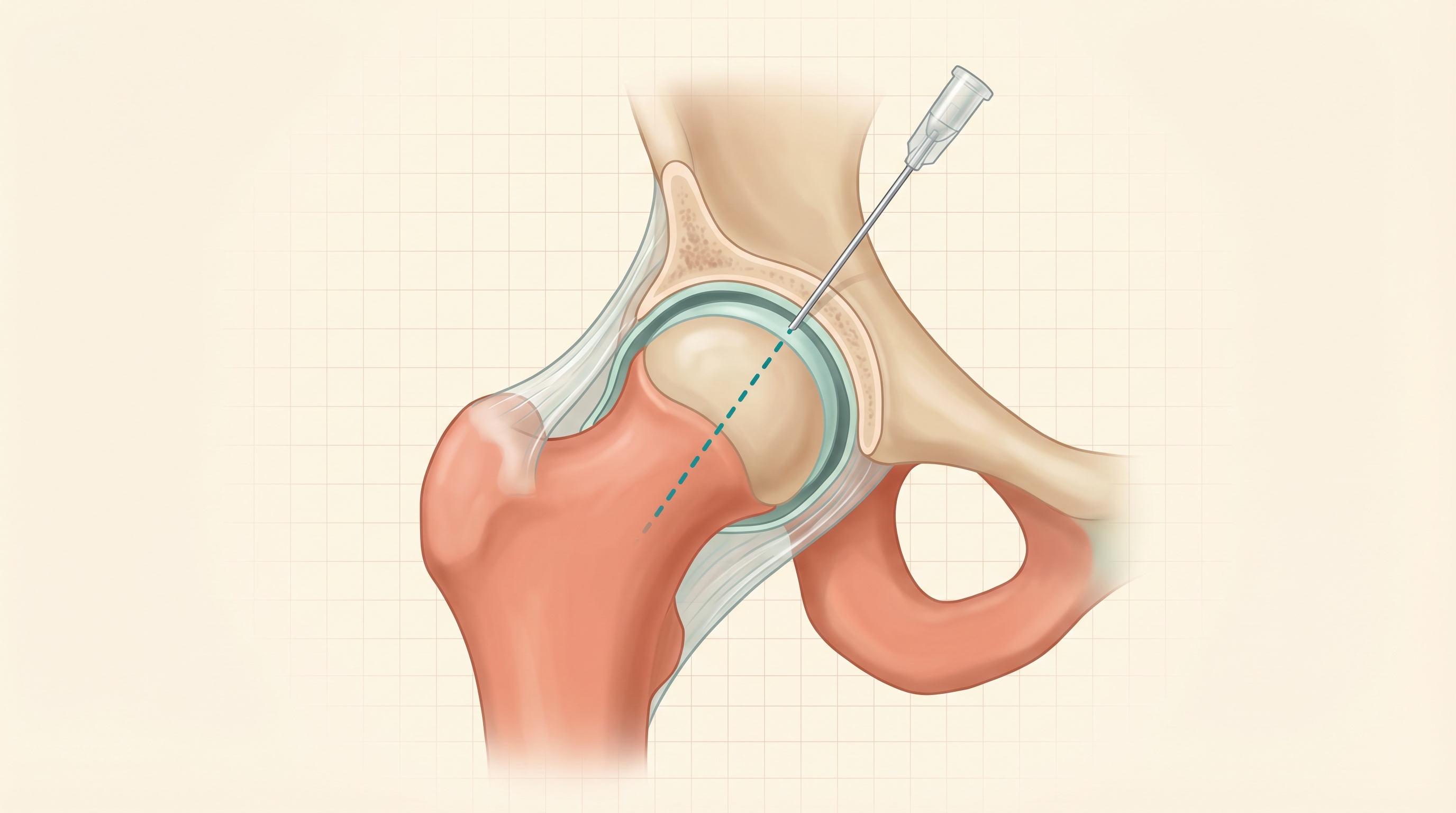
If you have had a knee injection before, you might assume hip injections work the same way. The procedures are similar in concept, but the hip has important anatomical differences that affect how injections are performed:
The Four Hip Injection Types Compared
| Factor | Cortisone | HA (Gel) | PRP | Stem Cell |
|---|---|---|---|---|
| FDA Status (Hip) | Approved | Off-label | Off-label | Experimental |
| Evidence Level | Strong | Moderate | Emerging | Insufficient |
| Relief Duration | 4-12 weeks | 3-6 months | 6-12 months (variable) | Unknown |
| Onset of Relief | 2-7 days | 2-4 weeks | 4-6 weeks | 4-8 weeks |
| Repeat Frequency | 3-4x per year max | Every 6 months | Every 6-12 months | Unclear |
| Medicare Covered | Yes | Varies by plan | No | No |
| Typical Cost | $50-$150 (with insurance) | $300-$800 | $500-$1,500 | $3,000-$8,000 |
| Imaging Needed | Strongly recommended | Yes | Yes | Yes |
Cortisone Injections for Hip Arthritis
Cortisone (corticosteroid) injections are the most commonly used hip injection and the typical starting point.
How It Works
A corticosteroid combined with a local anesthetic is injected directly into the hip joint. The steroid reduces inflammation, and the anesthetic provides immediate (temporary) pain relief while the steroid takes effect over 2-7 days.
What the Evidence Shows
Cost and Coverage
Medicare Part B covers cortisone hip injections. With supplemental insurance, your out-of-pocket cost is typically $50-$150 including the imaging guidance fee. Without insurance, expect $250-$500.
Hyaluronic Acid (Gel) Injections for Hip
HA injections restore the natural cushioning fluid in your joint. While FDA-approved only for the knee, their use in the hip has grown substantially based on positive research.
How It Works
A gel-like substance made of hyaluronic acid (the same material that naturally lubricates your joints) is injected into the hip joint. It supplements your depleted joint fluid, reducing friction and potentially providing anti-inflammatory effects.
What the Evidence Shows
Cost and Coverage
Medicare covers HA injections for the knee but not consistently for the hip. Some Medicare Advantage plans cover off-label hip use with prior authorization. Private insurance coverage varies. Without insurance, expect $300-$800 per injection or series.
Related reading: Gel Injections for Hip Arthritis
PRP Injections for Hip Arthritis
Platelet-rich plasma (PRP) uses concentrated growth factors from your own blood to reduce inflammation and potentially promote healing.
How It Works
Blood is drawn from your arm, spun in a centrifuge to concentrate the platelets and growth factors, then injected into the hip joint under imaging guidance. The entire process takes about 30-60 minutes.
What the Evidence Shows
Cost and Coverage
PRP is not covered by Medicare or most private insurance. Typical cost is $500-$1,500 per injection. Some patients require 2-3 injections for optimal results.
Stem Cell Therapy for Hip Arthritis
Stem cell injections represent the most experimental option currently marketed for hip arthritis.
How It Works
Stem cells are harvested from your bone marrow (usually from the pelvis) or fat tissue, processed, and injected into the hip joint. The theory is that these cells can reduce inflammation and potentially support cartilage repair.
What the Evidence Shows
Cost and Coverage
Not covered by any insurance. Costs range from $3,000-$8,000 per treatment. Be cautious of clinics requiring large upfront packages.
Related reading: Stem Cell Therapy for Joint Pain: What the Evidence Shows
Hip Treatment Research Updates
Get evidence-based information about hip arthritis treatments, new research, and insurance coverage changes delivered to your inbox.
Join 10,000+ readers. No spam.
Latest Evidence on Hip Arthritis Management (2025-2026)
Recent research has provided important updates for anyone managing hip arthritis with or without injections.
Injection Accuracy: The Numbers Are Stark
Published accuracy studies show just how much imaging guidance matters for the hip:
- Blind (landmark-guided) hip injections hit the joint only 50-80% of the time depending on the study and provider experience
- Ultrasound-guided hip injections achieve accuracy rates of 94-100%
If your hip injection did not work, there is a real chance the medication never reached the joint. Always ask whether your provider uses fluoroscopy or ultrasound guidance.
Conservative Treatment Delays Hip Replacement Significantly
A large outcomes study found that conservative management (injections, PT, weight loss, exercise) delays total hip replacement by 3-7 years in most patients. Even more encouraging: only 26% of hip OA patients needed surgery within 5 years of diagnosis when treated with a comprehensive conservative approach. This means three out of four patients can manage their hip arthritis without surgery for at least 5 years.
Aquatic Exercise Is the Most Effective Non-Surgical Intervention
Among all non-surgical treatments studied for hip arthritis, aquatic exercise produced the largest effect size (d=1.12) — which is classified as a large effect in clinical research. Water-based exercise reduces the weight on your hip by 50-90% while providing resistance for strengthening. If you have access to a pool, aquatic exercise should be a central part of your hip arthritis management plan.
Weight Loss Has a Powerful Impact
Research confirms that losing 10% of your body weight results in a 25-30% improvement in hip arthritis symptoms. For a 200-pound person, that means losing 20 pounds could reduce your pain and stiffness by roughly a quarter. Weight loss works alongside any injection treatment — it does not replace injections, but it makes them work better.
The best approach for most hip arthritis patients: Combine imaging-guided injections with aquatic exercise, land-based physical therapy, and gradual weight loss if applicable. This multimodal strategy gives you the best chance of delaying or avoiding hip replacement surgery.
Why Imaging Guidance Is Essential for Hip
This point cannot be overstated. The hip joint is surrounded by major blood vessels (femoral artery and vein) and nerves. Accurate needle placement requires visualization.
If your provider does not use imaging guidance for hip injections, ask why or seek a provider who does.
Choosing the Right Injection for You
Start with cortisone if:
- You have never had a hip injection before
- You need quick pain relief for an acute flare
- You want a diagnostic test to confirm the hip joint as your pain source
- Budget and insurance coverage matter
Consider HA (gel) injections if:
- Cortisone works but wears off too quickly
- You want longer-lasting relief (3-6 months vs. 4-12 weeks)
- You are concerned about repeated steroid effects on cartilage
- You are trying to delay hip replacement
Consider PRP if:
- You have not responded well to cortisone or HA
- You are willing to pay out-of-pocket
- You want to try a biologic, regenerative approach
- You are under 65 with mild to moderate arthritis
Think carefully about stem cells if:
- You have exhausted other injection options
- You understand the limited evidence
- You choose a provider conducting proper research, not a marketing-driven clinic
Frequently Asked Questions
Are hip injections painful?
Most patients describe hip injections as uncomfortable but tolerable. Local anesthetic numbs the skin and tissue before the deeper injection. With imaging guidance, the procedure takes about 5-10 minutes. Most people drive themselves home afterward.
How long does it take for a hip injection to work?
Cortisone typically provides relief within 2-7 days. HA (gel) injections take 2-4 weeks for full effect. PRP may take 4-6 weeks. If you do not notice improvement by the expected timeframe, contact your provider.
Can you get hip injections on blood thinners?
Yes, for cortisone and HA injections. Most guidelines say blood thinners do not need to be stopped for standard joint injections. PRP may require a temporary hold on certain blood thinners. Always inform your doctor about all medications.
How many hip injections can you get per year?
Cortisone is typically limited to 3-4 per year per joint. HA injections can be repeated every 6 months. PRP frequency is less standardized but usually every 6-12 months. There is no lifetime limit on cortisone or HA injections, but your doctor will reassess whether they continue to provide adequate benefit.
Does insurance cover hip injections?
Cortisone hip injections are covered by Medicare and most insurance. HA injections are covered for the knee by Medicare but coverage for the hip varies by plan since it is off-label. PRP and stem cell injections are not covered by any major insurance. Always verify with your specific plan before scheduling.
What happens if hip injections stop working?
If injections no longer provide meaningful relief, it usually means the arthritis has progressed beyond what injections can manage. This is a reasonable time to discuss surgical options with an orthopedic surgeon. Your documented injection history actually helps with surgical insurance authorization.
Is one hip injection brand better than others?
For HA injections, brands like Synvisc, Hyalgan, and Supartz have the most published data for hip use. Single-injection options (Synvisc-One, Gel-One, Monovisc) are popular for the hip since they minimize the number of imaging-guided procedures needed. Ask your provider which brand they have the most experience with.
This article is for informational purposes only and does not replace medical advice. Consult with your healthcare provider about the treatment plan that is right for your individual situation.
Last reviewed: March 2026
Related Resources
Topics
Enjoyed this article?
Get more insights like this delivered to your inbox weekly.
Join 10,000+ readers. No spam.