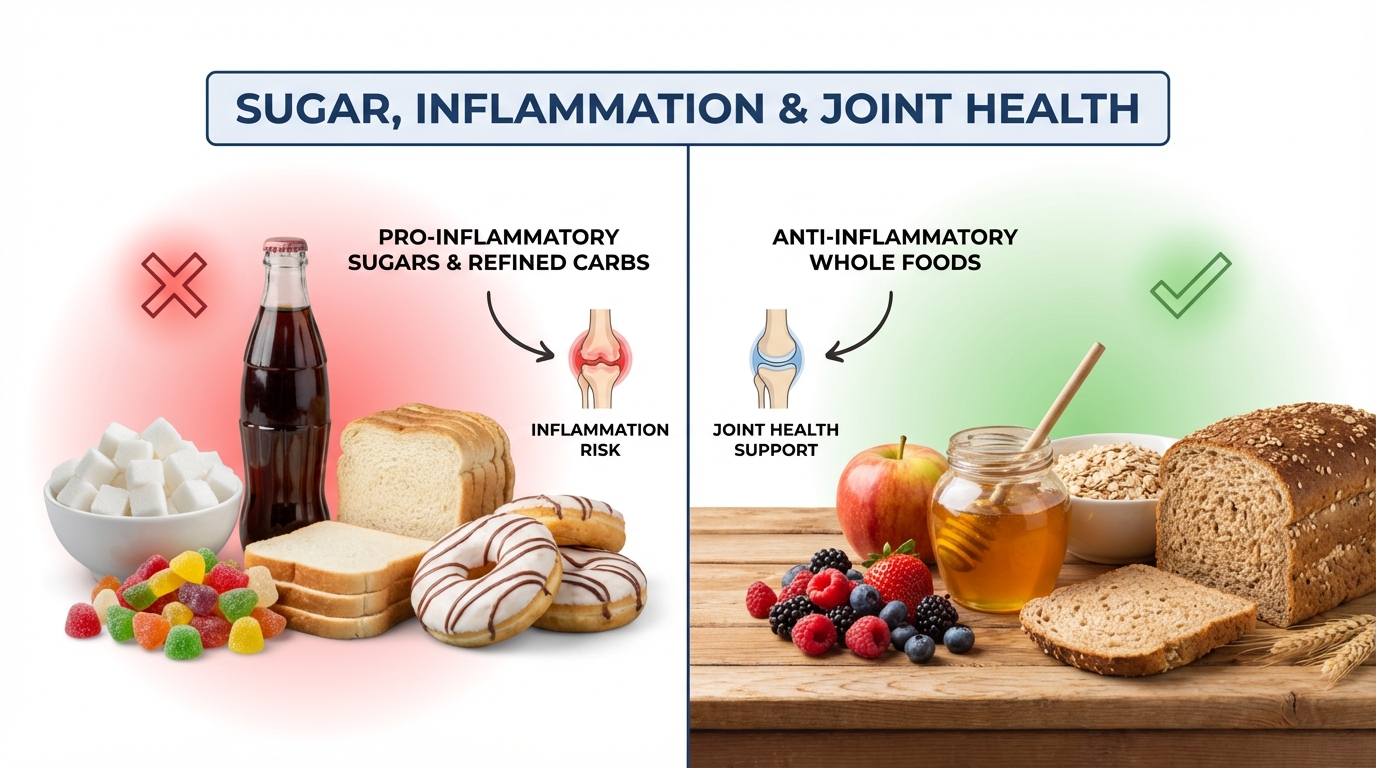
Sugar and Joint Pain: How Sweets Fuel Inflammation
Understand how sugar and refined carbs increase inflammation and worsen joint pain. Learn to spot hidden sugars and find satisfying alternatives.
By Joint Pain Authority Team
Key Takeaways
- Excess sugar triggers the release of inflammatory chemicals that damage joint cartilage
- The average American consumes about 17 teaspoons of added sugar daily—nearly triple the recommended limit
- Hidden sugars in processed foods, sauces, and “healthy” products are a major source
- Reducing sugar intake can lower inflammatory markers within weeks
- Satisfying alternatives exist that won’t spike your blood sugar or worsen your joints
If your joints ache more after a weekend of desserts or holiday treats, it’s not your imagination. Sugar and refined carbohydrates are among the most potent dietary triggers of inflammation, and that inflammation goes directly to your joints.
This doesn’t mean you can never enjoy a sweet treat. But understanding how sugar affects your joints—and where it hides in your daily diet—puts you in control. Small reductions in sugar intake can produce meaningful reductions in joint pain.
How Sugar Causes Joint Inflammation
When you eat sugar or refined carbohydrates (white bread, pastries, white rice), your blood sugar rises quickly. This triggers a cascade of events that increase inflammation throughout your body:
The Insulin-Inflammation Connection
High blood sugar signals your pancreas to release a surge of insulin. Repeated insulin spikes promote the production of inflammatory chemicals called cytokines—specifically IL-6, TNF-alpha, and CRP. These are the same inflammatory markers elevated in people with knee osteoarthritis, gout, and fibromyalgia.
Advanced Glycation End Products (AGEs)
When sugar molecules attach to proteins or fats in your body, they form compounds called AGEs (advanced glycation end products). AGEs accumulate in joint tissues and cause direct damage:
- They stiffen collagen in cartilage, making it brittle and less resilient
- They trigger inflammatory responses in joint lining tissues
- They increase oxidative stress that accelerates cartilage breakdown
AGEs accumulate with age, which is one reason joint problems worsen over time. A high-sugar diet dramatically accelerates this process.
Fructose and Uric Acid
Fructose (found in table sugar, high-fructose corn syrup, and excessive fruit juice) has a unique metabolic pathway that increases uric acid production. Elevated uric acid doesn’t just cause gout—it also promotes inflammation in non-gout arthritis and contributes to metabolic syndrome, which worsens osteoarthritis.
A study in The American Journal of Clinical Nutrition found that people who consumed the most fructose had significantly higher uric acid levels and inflammatory markers compared to those who consumed the least.
How Much Sugar Is Too Much?
The American Heart Association recommends:
- Women: No more than 6 teaspoons (25 grams) of added sugar daily
- Men: No more than 9 teaspoons (36 grams) of added sugar daily
For reference, a single can of regular soda contains about 10 teaspoons (39 grams) of sugar—already exceeding the daily limit.
The average American consumes about 17 teaspoons (71 grams) of added sugar daily. Much of this comes not from the sugar bowl, but from processed foods where sugar is hidden under various names.
Where Sugar Hides: The Sneaky Sources
Many people are surprised to learn how much sugar is in foods that don’t taste particularly sweet.
Common Hidden Sugar Sources
| Food Item | Added Sugar |
|---|---|
| Flavored yogurt (6 oz) | 4-6 teaspoons |
| Granola bar | 3-4 teaspoons |
| Pasta sauce (1/2 cup) | 2-3 teaspoons |
| Salad dressing (2 tbsp) | 1-2 teaspoons |
| Instant oatmeal packet | 3-4 teaspoons |
| Ketchup (2 tbsp) | 2 teaspoons |
| Barbecue sauce (2 tbsp) | 3-4 teaspoons |
| ”Healthy” smoothie (store-bought) | 6-10 teaspoons |
| Whole wheat bread (2 slices) | 1-2 teaspoons |
| Sports drink (20 oz) | 8-9 teaspoons |
Sugar’s Many Names on Labels
Sugar appears on ingredient lists under more than 60 different names. Watch for:
- High-fructose corn syrup
- Sucrose, glucose, fructose, dextrose, maltose
- Cane sugar, cane juice, evaporated cane juice
- Agave nectar, honey, maple syrup, molasses
- Brown rice syrup, corn syrup
- Fruit juice concentrate
- Maltodextrin
Rule of thumb: If a word ends in “-ose” or includes “syrup,” it’s sugar.
The Research: Sugar and Joint Pain
The connection between sugar and joint problems is well-documented:
- A large study published in Arthritis Care & Research found that regular consumption of sugar-sweetened soda was associated with increased risk of rheumatoid arthritis in women
- Research in the American Journal of Clinical Nutrition linked higher sugar intake to elevated CRP levels, a marker of systemic inflammation that correlates with arthritis severity
- A 2020 study showed that people with knee OA who consumed more added sugar had greater joint pain and faster cartilage deterioration
- For gout patients, a study in the British Medical Journal found that men who consumed 2 or more sugary sodas daily had an 85% higher risk of gout compared to men who rarely drank soda
Refined Carbohydrates: Sugar in Disguise
It’s not just the obviously sweet stuff. Refined carbohydrates—white bread, white rice, white pasta, crackers, and chips—convert rapidly to sugar in your blood. They cause the same insulin spikes and inflammatory cascades as eating sugar directly.
The glycemic index (GI) measures how quickly foods raise blood sugar. High-GI foods to reduce:
| High-GI (Reduce) | Low-GI (Better Choice) |
|---|---|
| White bread | Whole grain or sourdough bread |
| White rice | Brown rice, quinoa, barley |
| Regular pasta | Whole wheat pasta, lentil pasta |
| Instant oatmeal | Steel-cut or rolled oats |
| Potato chips | Nuts, seeds, raw vegetables |
| Pretzels | Whole grain crackers with cheese |
| Sugary cereal | Plain oatmeal with berries |
How to Reduce Sugar Without Feeling Deprived
Cutting sugar cold turkey is difficult and often leads to cravings and rebound. A gradual approach works better for lasting change.
Week 1-2: Eliminate Sugary Drinks
This single change can remove 15-20 teaspoons of sugar daily for some people. Replace with:
- Water (plain or infused with fruit slices)
- Sparkling water with a squeeze of lemon or lime
- Unsweetened iced tea
- Unsweetened tart cherry juice diluted with water (bonus: anti-inflammatory benefits)
Week 3-4: Swap Breakfast
Replace sugary cereals, pastries, and flavored yogurt with:
- Steel-cut oatmeal with walnuts and fresh berries (natural sweetness)
- Plain Greek yogurt with a drizzle of honey and sliced fruit
- Eggs with vegetables and whole grain toast
- Smoothie made with plain yogurt, frozen berries, and ground flaxseed
Week 5-6: Audit Sauces and Condiments
Check labels and swap high-sugar options:
- Replace ketchup with mustard or salsa
- Make simple salad dressings with olive oil, vinegar, and herbs
- Choose marinara sauce with less than 5 grams sugar per serving
- Use spices and herbs to add flavor instead of sweet sauces
Week 7-8: Address Snacking
Replace candy, cookies, and processed snacks with:
- Fresh fruit with nut butter
- A handful of walnuts or almonds
- Cheese with whole grain crackers
- Hummus with raw vegetables
- Dark chocolate (70%+ cocoa, 1-2 small squares—much less sugar than milk chocolate)
Natural Sweetener Alternatives
When you need sweetness, some options are better than refined sugar:
Better choices:
- Fresh fruit provides sweetness plus fiber, vitamins, and antioxidants
- Cinnamon adds natural sweetness to oatmeal, yogurt, and coffee without sugar
- Vanilla extract enhances perceived sweetness in baked goods
- Small amounts of honey or maple syrup provide some beneficial compounds alongside their sugar
Use cautiously:
- Stevia and monk fruit are calorie-free and don’t spike blood sugar, but some people dislike the taste
- Artificial sweeteners don’t raise blood sugar but may disrupt gut bacteria, which also affects joint inflammation
What to Expect When You Cut Back
Days 1-3: You may experience cravings, headaches, and irritability as your body adjusts. This is normal and passes.
Week 1-2: Cravings begin to diminish. You may notice improved energy levels and steadier mood.
Week 3-4: Your taste buds recalibrate. Foods you never noticed as sweet (like carrots, bell peppers, berries) start tasting sweeter. Former favorites may taste overwhelmingly sweet.
Week 6-8: Many people report less morning stiffness, reduced joint swelling, and improved pain levels. Inflammatory markers like CRP typically decrease within this timeframe.
Long-term: Consistent low-sugar eating becomes your new normal. The combination of lower inflammation, potential weight loss, and better overall health compounds the joint benefits over months and years.
Sugar Reduction and Medical Treatment
If you’re taking oral medications for joint pain, reducing sugar intake can enhance their effectiveness. Less systemic inflammation means your medications work in a less hostile environment. Some patients find they can eventually reduce their medication needs in consultation with their doctor.
For people with gout, sugar reduction is particularly important alongside medication. Lower fructose intake directly reduces uric acid production, complementing drugs like allopurinol that reduce uric acid through a different mechanism.
Frequently Asked Questions
Will cutting sugar completely eliminate my joint pain?
No. Sugar reduction is one piece of a larger puzzle. It can meaningfully reduce inflammation and improve symptoms, but arthritis involves structural changes in your joints that diet alone cannot fully address. Sugar reduction works best alongside appropriate medical care and other lifestyle changes.
Is fruit sugar bad for my joints too?
Whole fruits are fine and even beneficial. They contain fiber that slows sugar absorption, plus anti-inflammatory vitamins and antioxidants. The concern is with added sugars, fruit juice (where the fiber is removed), and concentrated sweeteners. Enjoy 2-3 servings of whole fruit daily without worry.
How much sugar reduction is needed to make a difference?
Even cutting your added sugar intake by half can produce noticeable results. If you currently consume the American average of 17 teaspoons daily, getting down to 6-9 teaspoons would represent a significant anti-inflammatory shift. Start with the biggest sources (sugary drinks, desserts) for the greatest impact.
Are sugar-free products a good alternative?
Some can be helpful, but read labels carefully. Many sugar-free products contain artificial sweeteners that may disrupt gut health, or they add extra fat or salt to compensate for lost sweetness. The best approach is to choose whole, naturally low-sugar foods rather than processed “sugar-free” substitutes.
Does sugar cause arthritis, or does it just make it worse?
Sugar doesn’t cause osteoarthritis directly—wear, tear, genetics, and aging are the primary factors. However, chronic high sugar intake promotes systemic inflammation and AGE formation that accelerate cartilage damage and worsen symptoms. For gout, fructose directly increases uric acid, which can trigger the disease in susceptible people.
The information in this article is for educational purposes only and is not intended as medical advice. Always consult with your healthcare provider before making significant dietary changes, especially if you have diabetes or take blood sugar-regulating medications.
Last medically reviewed: February 2026
Topics
Enjoyed this article?
Get more insights like this delivered to your inbox weekly.
Join 10,000+ readers. No spam.